KHealth: Semantic Multisensory Mobile Approach to Personalized Asthma Care
Contents
- 1 Motivation and Background
- 2 kHealth Vision
- 3 kHealth: Knowledge-enabled Personalised Digital Healthcare
- 4 Asthma: Challenges and Opportunities
- 5 kHealth for Asthma
- 6 Funding
- 7 People
- 8 Related kHealth Projects
- 9 kHealth Observations
- 10 Preliminary Data Analysis
- 11 IRB
- 12 kHealth User Manual
- 13 kHealth App Introduction
- 14 Related Talks and Presentations
- 15 Chatbot for Asthma Management
- 16 Acknowledgement
- 17 Publications
- 18 Concurrent Projects
- 19 References
Motivation and Background
More than 25 million people in the U.S. are diagnosed with asthma, out of which 7 million are children [1]. Asthma related healthcare costs alone are around $50 billion a year [2]. Current reactive healthcare costs more than 17% of GDP in the US [3, 4]. Specifically, with the current reactive care for asthma, there were 155,000 hospital admissions and 593,000 ER visits in 2006 [16]. It is estimated that, by 2025, over 400 million people will be affected by asthma worldwide. With increasing adoption of mobile devices and low-cost sensors, an unprecedented amount of data is being collected by people [5]. This data collection has exacerbated the problem of understanding the data and making sense of it. In this project, we explore the role of knowledge empowered algorithms in making sense of this data deluge in the context of asthma assessment and management.
kHealth Vision
Digital health and mobile health applications are benefiting from semantic web research from Wright State's Ohio Center of Excellence in Knowledge-Enabled Computing (Kno.e.sis). Director of Kno.e.sis and Professor of Computer Science and Engineering Dr. Amit Sheth describes the development of mobile health applications with sensor technology to monitor patient health, mobile computational support, and clear feedback to the patient and physician.
Amit Sheth, Pramod Anantharam, Krishnaprasad Thirunarayan, "kHealth: Proactive Personalized Actionable Information for Better Healthcare", Workshop on Personal Data Analytics in the Internet of Things at VLDB2014, Hangzhou, China, September 5, 2014.
Keynote at WorldComp2014, July 21, 2014. Smart Data for you and me: Personalized and Actionable Physical Cyber Social Big Data.
kHealth: Knowledge-enabled Personalised Digital Healthcare
Augmented Personalized Healthcare (APH) is expected to enhance healthcare by personalizing the use of all relevant physical, cyber, and social data [2] obtained from wearables, sensors and Internet of Things (IoT), mobile applications, Electronic Medical Records (EMRs), web-based information, and social media. The exploitation of all relevant data, relevant medical knowledge, and AI techniques will extend and enhance human health and well-being. The concept of augmentation refers to the aggregation and integration of all the signals at the personal, public and population level obtained by analyzing data and knowledge from sensors and the Web that can affect human health, and then converting these signals and data into actions that improve health-related outcomes. These signals collected both passively (without patient engagement) and actively (with patient or physician engagement) can help make better and more timely decisions. This embodiment of APH is an entirely new approach to human health compared to the current episodic system of periodic care primarily centered around healthcare establishments (such as clinics, hospitals, and labs). APH involves continuous monitoring, engagement, and health management, where rather than treating a patient with a disease, the focus shifts to involving the patient in preventing disease, predicting possible adverse outcomes and preventing them through proactive measures, and keeping them healthy and fit with lifestyle changes. Rather than chronic disease management, it takes a holistic approach to improving the overall quality of life.
Asthma: Challenges and Opportunities
Asthma is a great example of a problem that spans Physical-Cyber-Social (PCS) systems. The health signals related to asthma spans Physical (environmental), Cyber (CDC reports), and Social (asthma/symptom reports on social media) modalities. Specifically, for asthma, we group health signals as personal (wheezing level, exhaled Nitric Oxide), population (asthma reports on social media), and public health signals (CDC asthma reports).

kHealth for Asthma
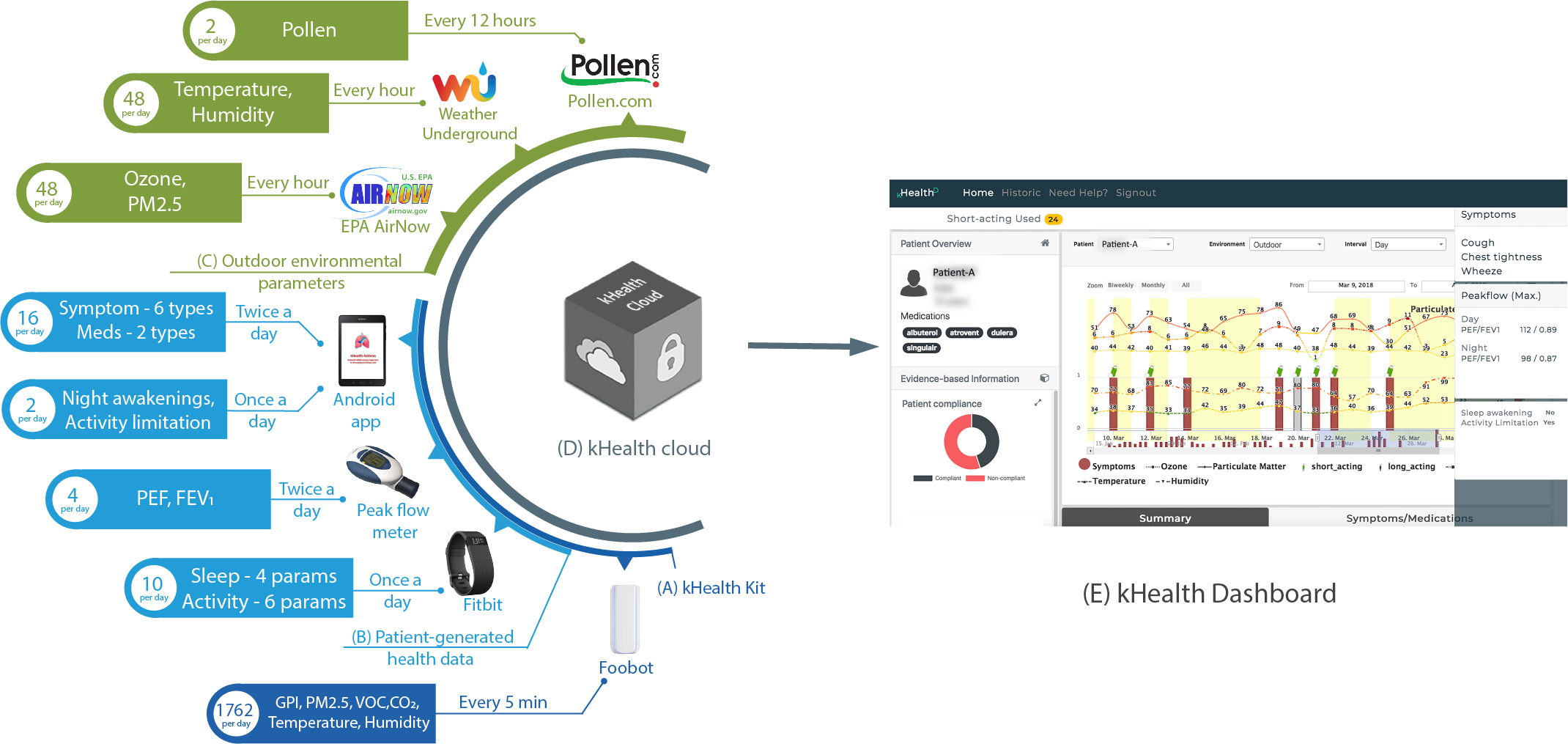
We tackle this important problem by a combination of active and passive sensing. Active sensing involves the patient in the loop (obtrusive) while passive sensing does not involve patient involvement (unobtrusive). Using a novel approach of utilizes low-cost sensors for continuous monitoring (active and passive sensing), we propose to develop algorithms that can take this multi-modal data and translate them to practical and actionable information for asthma patients and their healthcare provider. Specifically, provide information on asthma control level based on symptoms and their severity, asthma triggers and early alerts for increasing asthma symptoms. The kHealth-Asthma consist of kHealth kit, kHealth cloud, and kHealth Dashboard. kHealth Dashboard shows the frequency of data collection, the number of parameters collected, and the total number of data points collected per day per patient. (A) Dark blue; the kHealth kit components that are given to the patient. (B) Light blue; the kHealth kit components that collect patient-generated health data. (C) Green; the outdoor environmental parameters and their sources. (D) The kHealth cloud (gray). (E) The kHealth Dashboard. All kHealth data are anonymized and associated with respective randomly assigned patient IDs. FEV1: forced expiratory volume in 1 second; PEF: peak expiratory flow; PM2.5: particulate matter.
Funding
|
|
|
People
- Principal Investigators:
- Dr. Amit P. Sheth (Kno.e.sis, Wright State University)
- Co-Investigators
- Dr. T.K.Prasad (Kno.e.sis, Wright State University)
- Dr. Tanvi Banerjee (Kno.e.sis, Wright State University)
- Dr. Maninder Kalra (Dayton Children Hospital)
- Graduate Students from Kno.e.sis, Wright State University:
- Alumni:
Contact: Utkarshani Jaimini <html><center><img src="https://raw.githubusercontent.com/JINU98/multisensory/main/4.jpg"></img></center></html> Left to right: Swati Padhee, Utkarshani Jaimini, Dr. T.K. Prasad, Dr. Amit Sheth, Dr. Maninder Kalra, Dr. Tanvi Banerjee, and Vaikunth Sridharan.
Related kHealth Projects
- KHealth Asthma Ontology (KAO)
- Augmented Personalized Health
- kHealth for Bariatric
- kHealth overview with example of ADHF
- kHealth for dementia
- kHealth for reducing liver cirrhosis readmission (to come)
kHealth Observations
Asthma is a multi-faceted problem and we propose a holistic solution for
Personal
Physiological: Wheezometer [6], Nitric Oxide [7], Accelerometer, Microphone, Contextual Questions
Environmental: Foobot [17], Sensordrone [8], Dust Sensor [9], Location
Public Health
CDC [10], DCHC’s EMR Records (periodic manual review)
Population Level
Everyaware [11], AirQuality Egg [12], Allergy Alerts [13,14], Social Observations (e.g., tweets), Air Quality Index[15]
Preliminary Data Analysis
kHealth kit could be used to collect observations (both sensor and patients questionnaire response) in the patient home environment (which was never accessible in a quantitative form to doctors). These observations when collected based on expert guidance, prove valuable for clinical decision support. These observations when interpreted by a doctor, lead to some interesting insights:
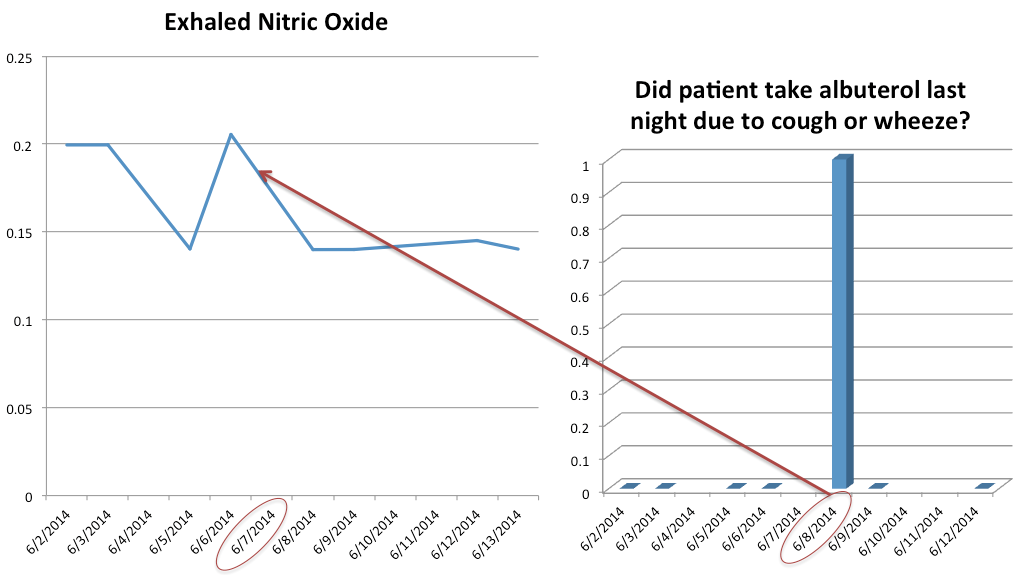
*Activity limitation is likely related to high exhaled Nitric Oxide
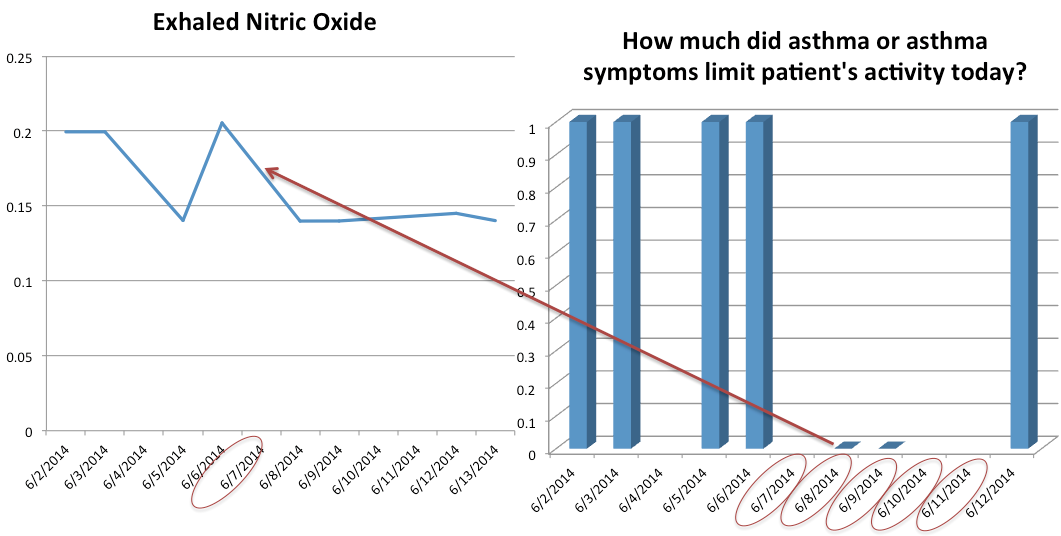
*Low exhaled Nitric Oxide observed with absence of coughing
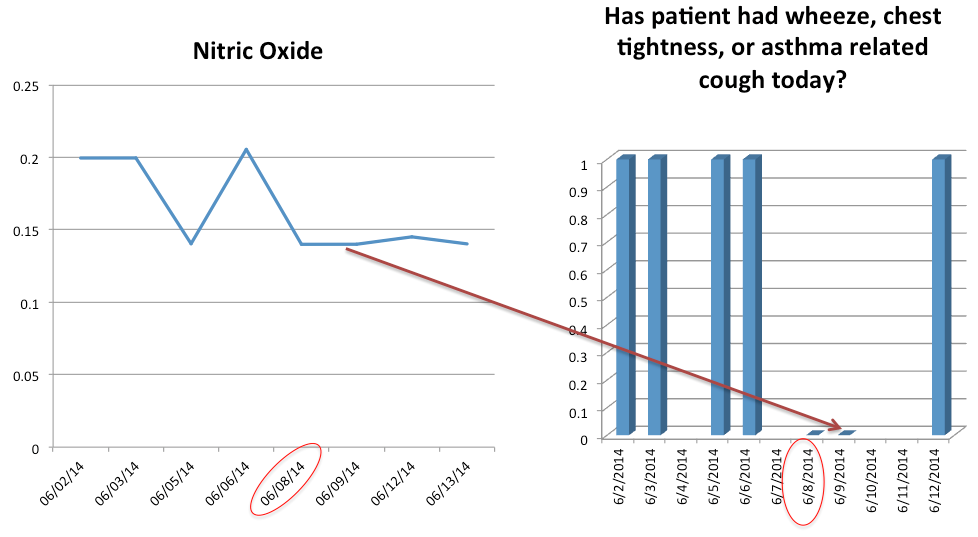
*Activity limitation observed with high pollen activity
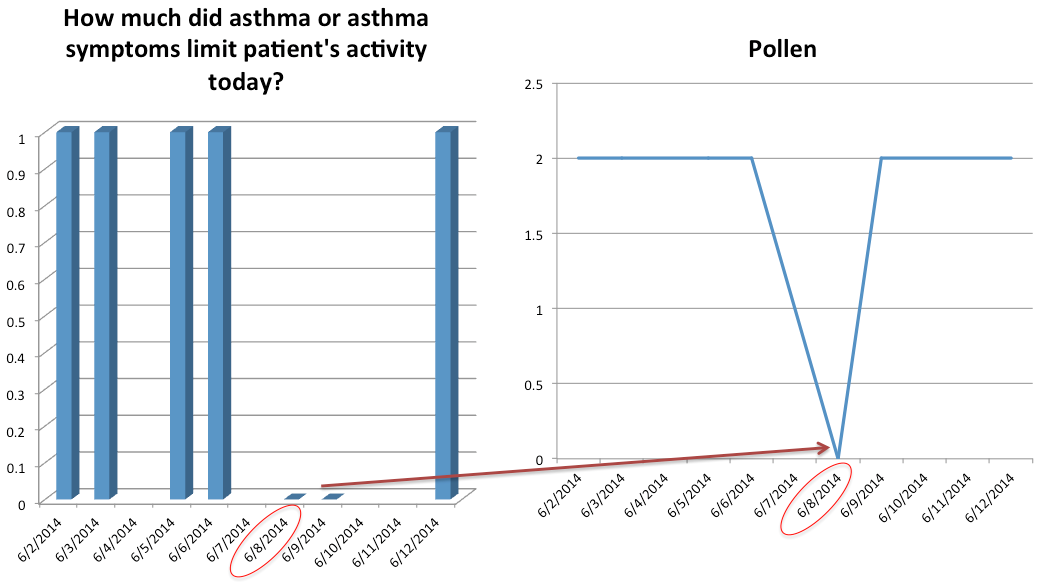
THESE PRELIMINARY FINDINGS NEED TO BE VALIDATED IN LARGER STUDIES
Dataset Size
We collect observations from three sensors (temperature, humidity, Carbon monoxide) on Sensordrone at the rate of 1 Hz (1 observation/second). Nitric Oxide observations from the NODE sensor are collected at the rate of 2 observations/day. Patients answer a questionnaire which has 5 questions resulting in 5 observations/day. For a single patient, we collect over 250,000 observations/day. In our study of three patients, we have collected over 9 million data points.
Foobot Reliability Testing
We used an indoor air quality monitor, Foobot to monitor patient's indoor environment. Foobot measure five different air quality parameters (with thresholds defined by Foobot): Particulate Matter (25 ug/m3), Volatile Organic Compounds (300 ppb), Carbon Dioxide (1300 ppm), Temperature (40 celsius), Relative Humidity(60%). It records data every 5 minutes. The Foobot has been used in many medical facilities and its calibration is checked at regular intervals.
In terms of system error measurement, the following specifications were provided by the manufacturer:
1. Particulate Matter (PM) - Detection range 0 to 1 300 µg/m³ ; Precision ±4µg or ±20%
2. Volatile Organic Compounds (VOC) - Detection range: 100 to 1000 ppb
3. Carbon Dioxide - Detection range 400-6000 ppm
4. Temperature - Detection range 15 to 45°C; ±1°C
5. Humidity - Detection range 30 to 85% (non-condensing) ; RH ±5%
To further test the reliability of the Foobot devices, we tested three Foobot sensors concurrently in two different environments.
(i) The first experiment was intended to model the consistency of the Foobot in a relatively clean, controlled environment. (ii)The second was intended to model the type of consistency that might be expected in an environment where polluting activity such as cooking or smoking is occurring.
To test consistency in a clean, controlled environment, we put four Foobots in an unused office for a duration of three hours. Data were recorded at 5-minute intervals by each device over this time period. Using a two-way main effects ANOVA model which included Sensor and Time as fixed factors, we quantified the average between-sensor consistency across time using the sensor-specific root mean square deviation (RMSD). We also used the sensor-specific RMSD to quantify between-sensor consistency in the cooking environment by placing three sensors in a kitchen where cooking (stir fry) was happening. The sensors were placed at a distance of 10 meters from the cooking event. Two cooking events were measured. The first was approximately was approximately 2.5 hours duration, and the second was a 40-minute duration. The sensor-specific RMSD was quantified through a 3-way factorial ANOVA model, where Time, Cooking Event, and Sensor, were treated as fixed factors.
In the controlled environment, PM and VOC showed no variation. While this is indicative of a relatively clean and unchanging environment, it was difficult to get a reliable estimate of the precision of these measures. In the cooking environment, both the ranges and average differences between sensors were larger. Through the two cooking events, PM ranged from 0 to 68.3, with a RMSD of 12.33. This amounts to an average percent error of around 20%. VOC ranged from 125.0 to 242.0, with an RMSD of 23.35, which indicates a percent error of 10-19%. In the controlled environment, average carbon dioxide levels ranged between 450.0 and 451.0, with an average difference between sensors of 0.98, which amounts to a percent error below 0.3%. The range increased to 450.0-875.0, and the RMSD increased to 85.31, amounting to a percent error of 10-19%. The significantly larger error rates in PM, VOC, and carbon dioxide during the cooking event results from the increased variation of PM and VOC in the environment, and the fact that PM and VOC are distributed unevenly in the room. It is likely that much of between-device difference is due to different concentration gradients of PM, VOC, and carbon dioxide in the environment. While this is not indicative of a limitation of the device itself, it does show that the concentration of these chemicals may be different between the location of the device and the patient. To the end of monitoring air quality toward reduction of asthma symptoms, this warrants a recommendation to keep the device as close to the patient as possible.
Unlike PM, VOC, and carbon dioxide, temperature and humidity measures are consistent and precise in both the controlled and Cooking environments. In the controlled environment, the temperature ranged from 21.69 to 22.34 C, and the RMSD between devices was 0.96. This yielded a percent error below 5%. Percent error dropped below 3% in the Cooking environment, where temperatures ranged between 18.74 and 27.38 C, with and RMSD of 0.53. For measurement of humidity, percent error rates were below 10% for both the controlled and Cooking environments. In the controlled environment, humidity ranged between 27.83 and 29.08, with RMSD of 2.42. In the Cooking environment, values ranged between 30.47 and 46.83, with and RMSD of 2.04.
IRB
Dayton Children's Hospital Institutional Review Board (IRB) approved the pilot study in October 2013 which began enrolling pediatric patients and their parents to use the kHealth kit for Asthma. IRB continuation was approved in October 2014. Please contact Prof. Amit Sheth [amit at knoesis.org] or Dr. Shalini Forbis [ForbisS at childrensdayton.org] to obtain the exact copy of IRB.
kHealth User Manual

kHealth Asthma user guide link=https://drive.google.com/open?id=0Bx89F-t526J2UlFBUnJUUWJjb2M
kHealth App Introduction
Related Talks and Presentations
Chatbot for Asthma Management
Asthma, chronic pulmonary disease, is one of the major health issues in the United States. Given its chronic nature, the demand for continuous monitoring of patient’s adherence to the medication care plan, assessment of their environment triggers, and management of asthma control level can be challenging in traditional clinical settings and taxing on clinical professionals. A shift from a reactive to a proactive asthma care can improve health outcomes and reduce expenses. On the technology spectrum, smart conversational systems and Internet-of-Things (IoTs) are rapidly gaining popularity in the healthcare industry. By leveraging such technological prevalence, it is feasible to design a system that is capable of monitoring asthmatic patients for a prolonged period and empowering them to manage their health better. In this thesis, we describe kBot, a knowledge-driven personalized chatbot system designed to continuously track medication adherence of pediatric asthmatic patients (age 8 to 15) and monitor relevant health and environmental data. The outcome is to help asthma patients self manage their asthma progression by generating trigger alerts and educate them with various self-management strategies. kBOT takes the form of an Android application with a frontend chat interface capable of conversing both text and voice-based conversations and a backend cloud-based server application that handles data collection, processing, and dialogue management. The domain knowledge component is pieced together from the Asthma and Allergy Foundation of America, Mayoclinic, and Verywell Health as well as our clinical collaborator. Whereas, the personalization aspect is derived from the patient’s history of asthma collected from the questionnaires and day-to-day conversations. The system has been evaluated by eight asthma clinicians and eight computer science researchers for chatbot quality, technology acceptance, and system usability. kBOT achieved an overall technology acceptance score of greater than 8 on an 11-point Likert scale and a mean System Usability Score (SUS) greater than 80 from both evaluation groups.
Acknowledgement
This work is supported by National Institutes of Health under the Grant Number 1 R01 HD087132-01: KHealth: Semantic Multisensory Mobile Approach to Personalized Asthma Care. The content of this paper is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Publications
- Utkarshani Jaimini, Amit Sheth, Krishnaprasad Thirunarayan, Maninder Kalra, and Marco Valtorta, 2020. "Is It Safe for My Child’s Asthma?" 6th International Conference on Computational Social Science, IC2S2.
- Amit Sheth, Hong Yung Yip, Saeedeh Shekarpour. Extending Patient-Chatbot Experience with Internet-of-Things and Background Knowledge: Case Studies with Healthcare Applications. IEEE Intelligent Systems 34.4 (2019): 24-30.
- Amit Sheth, Hong Yung Yip, Arun Iyengar, Paul Tepper.Cognitive services and intelligent chatbots: current perspectives and special issue introduction. IEEE Internet Computing, 23(2), 6-12.
- Dipesh Kadariya, Revathy Venkataramanan, Hong Yung Yip, Maninder Kalra, Krishnaprasad Thirunarayan, Amit Sheth. "kBot: Knowledge-enabled Personalized Chatbot for Asthma Self-Management". In Proceedings of the IEEE SMARTSYS Workshop on Smart Service Systems (SMARTCOMP 2019). IEEE, 2019.
- Amit Sheth, Hong Yung Yip, Arun Iyengar, Paul Tepper. Cognitive Services and Intelligent Chatbots: Current Perspectives and Special Issue Introduction. IEEE Internet Computing, 23 (2), March-April 2019.
- Revathy Venkataramanan, Krishnaprasad Thirunarayan, Utkarshani Jaimini, Dipesh Kadariya, Hong Yung Yip, Maninder Kalra, Amit Sheth. Determination of Personalized Asthma Triggers from Multimodal Sensing and Mobile Application.,JMIR Pediatr Parent 2019;2(1):e14300 DOI: 10.2196/14300. PMCID: PMC6716491 PMID:31518318
- Utkarshani Jaimini, Krishnaprasad Thirunarayan, Maninder Kalra, Revathy Venkataramanan, Dipesh Kadariya, Amit Sheth. “How Is My Child’s Asthma?” Digital Phenotype and Actionable Insights for Pediatric Asthma., JMIR Pediatr Parent 2018;1(2):e11988, DOI: 10.2196/11988. PMCID: PMC6469868 NIHMSID: NIHMS1006255 PMID: 31008446
- Vaikunth Sridharan, Revathy Venkataramanan, Dipesh Kadariya, Krishnaprasad Thirunarayan, Amit Sheth, Maninder Kalra. “Knowledge-Enabled Personalized Dashboard for Asthma Management in Children”, Annals of Allergy, Asthma & Immunology 121.5 (2018): S42.
- Amelie Gyrard, Manas Gaur, Krishnaprasad Thirunarayan, Amit Sheth and Saeedeh Shekarpour. Personalized Health Knowledge Graph. 1st Workshop on Contextualized Knowledge Graph (CKG) co-located with International Semantic Web Conference (ISWC), 8-12 October 2018, Monterey, USA.
- Mahda Noura, Amelie Gyrard, Sebastian Heil, Martin Gaedke. Automatic Knowledge Extraction to build Semantic Web of Things Applications. IEEE Internet of Things (IoT) Journal 2019.
- Amit Sheth, Hong Yung Yip, Utkarshani Jaimini, Dipesh Kadariya, Vaikunth Sridharan, Revathy Venkataramanan, Tanvi Banerjee, Krishnaprasad Thirunarayam, Maninder Kalra. Feasibility of Recording Sleep Quality And Sleep Duration Using Fitbit in Children with Asthma Abstract in the 32nd Annual Meeting of the Associated Professional Sleep Societies (SLEEP), 2-6 June 2018, Baltimore, MD.
- Amit Sheth, Hong Yung Yip, Utkarshani Jaimini, Dipesh Kadariya, Vaikunth Sridharan, Revathy Venkataramanan, Tanvi Banerjee, Thirunarayam K, Maninder Kalra. Augmented Personalized Health: Using Semantically Integrated Multimodal Data for Patient Empowered Health Management Strategies. mHealth Technology Showcase, National Institute of Health- June 2018.
- Utkarshani Jaimini, Hong Yung Yip, Revathy Venkataramanan, Dipesh Kadariya, Vaikunth Sridharan, Tanvi Banerjee, Krishnaprasad Thirunarayan, Maninder Kalra, Amit Sheth. kHealth Digital Personalized Healthcare technology for Pediatric Asthma. mHealth Technology Showcase, National Institute of Health- June 2018.
- Amit P. Sheth, Tanvi Banerjee, Utkarshani Jaimini, Dipesh Kadariya, Vaikunth Sridharan, Krishnaprasad Thirunarayan, Revathy Venkataramanan, Hong Yung Yip, Maninder Kalra. Correlating Multimodal Signals with Asthma Control in Children Using kHealth Personalized Digital Health System. 2018.
- Amelie Gyrard, Antoine Zimmermann and Amit Sheth. Building IoT based applications for Smart Cities: How can ontology catalogs help?. IEEE Internet of Things Journal 2018
- Mahda Noura, Amelie Gyrard, Sebastian Heil and Martin Gaedke. Concept extraction from the web of things knowledge bases. International Conference WWW/Internet. 21-23 October 2018, Budapest, Hungary
- Amelie Gyrard, Manas Gaur, Swati Padhee, Amit Sheth and Mihaela Juganaru-Mathieu. Knowledge Extraction for the Web of Things (KE4WoT): WWW 2018 Challenge Summary. WWW '18 Companion Proceedings of The Web Conference, 23-27 April 2018, Lyon, France
- Paul Groth, Amelie Gyrard. Demo Track Chairs' Welcome & Organization. WWW '18 Companion Proceedings of The Web Conference 2018. 23-27 April 2018, Lyon, France
- Amit Sheth, Utkarshani Jaimini, Hong Yung Yip. How Will the Internet of Things Enable Augmented Personalized Health?. IEEE Intelligent Systems. IEEE; 2018 ;33(1).
- Amit Sheth, Sujan Perera, Sanjaya Wijeratne, Krishnaprasad Thirunarayan. "Knowledge will Propel Machine Understanding of Content: Extrapolating from Current Examples". In 2017 IEEE/WIC/ACM International Conference on Web Intelligence (WI). Leipzig, Germany: ACM; 2017. p. 1-9.
- Amit Sheth, Utkarshani Jaimini, Krishnaprasad Thirunarayan, Tanvi Banerjee. Augmented Personalized Health: How Smart Data with IoTs and AI is about to Change Healthcare. In 2017 IEEE 3rd International Forum on Research and Technologies for Society and Industry (RTSI 2017). Modena, Italy; 2017.
- Utkarshani Jaimini, Tanvi Banerjee, William Romine, Krishnaprasad Thirunarayan, Amit Sheth. Investigation of an Indoor Air Quality Sensor for Asthma Management in Children. In IEEE Sensors Letters, Volume 1, Issue 2, April 2017.
- Amit Sheth. Ontology-enabled Healthcare Applications Exploiting Physical-Cyber-Social Big Data. In Ontology Summit 2016. Virtual; 2016.
- Pramod Anantharam, Tanvi Banerjee, Amit Sheth, Krishnaprasad Thirunarayan, Surendra Marupudi, Vaikunth Sridharan, Shalini Forbis. Knowledge-driven Personalized Contextual mHealth Service for Asthma Management in Children. 2015 IEEE International Conference on Mobile Services. New York, NY: IEEE; 2015. p. 284 - 291.
- Amit Sheth. Smart Data: How You and I Will Exploit Big Data for Personalized Digital Health and Many Other Activities. 2015.
- Amit Sheth, Pramod Anantharam, Krishnaprasad Thirunarayan, "kHealth: Proactive Personalized Actionable Information for Better Healthcare", Workshop on Personal Data Analytics in the Internet of Things at VLDB2014, Hangzhou, China, September 5, 2014.
Concurrent Projects
- Modeling Social Behavior for Healthcare Utilization in Depression
- Augmented Personalized Healthcare
- Context-Aware Harassment Detection on Social Media (NSF)
- Hazards SEES: Social and Physical Sensing Enabled Decision Support for Disaster Management and Response (NSF)
- Project Safe Neighborhood
- eDrugTrends (NIH)
- Innovative NIDA National Early Warning Sysetm Network (iN3)
- MIDAS
- Market Driven Innovations and Scaling up of Twitris
References
- NHLBI description of Asthma, Available online at: http://www.nhlbi.nih.gov/health/health-topics/topics/asthma/
- Asthma related facts, Available online at: http://www.lung.org/lung-disease/asthma/resources/facts-and-figures/asthma-in-adults.html
- Squires, D. A., The U.S. Health System in Perspective: A Comparison of Twelve Industrialized Nations, June 2011, Available online at: http://bit.ly/oZwhFZ
- Health Costs: How the U.S. Compares With Other Countries, Available online at: http://www.pbs.org/newshour/rundown/2012/10/health-costs-how-the-us-compares-with-other-countries.html
- Quantified Self http://quantifiedself.com/
- Wheezometer by iSonea, Available online at: http://www.isoneamed.com/wheezometer.html
- Nitric Oxide Sensor, Available online at: http://nodesensors.com/product/oxa-gas-sensor-nitric-oxide-no/
- Sensordrone, a bluetooth enabled low-cost sensor for monitoring the environment, Available online at: http://www.kickstarter.com/projects/453951341/sensordrone-the-6th-sense-of-your-smartphoneand-be/
- Optical Dust Sensor, Available online at: https://www.sparkfun.com/products/9689
- Centers for Disease Control and Prevention, Available online at: http://www.cdc.gov/
- Everyaware, Sensing Air Pollution, Available online at: http://www.everyaware.eu/activities/case-studies/air-quality/
- Community-led sensing of AirQuality, Available online at: http://airqualityegg.com/
- National and Local Allergy Forecast, Available online at: http://www.pollen.com/allergy-weather-forecast.asp
- National Allergy Bureau Alerts, Available online at: http://www.aaaai.org/global/nab-pollen-counts.aspx
- Air Quality Index from United States Environmental Protection Agency, Available online at : http://www.epa.gov/
- Akinbami et al. (2009). Status of childhood asthma in the United States, 1980–2007. Pediatrics,123(Supplement 3), S131-S145.
- Foobot, Available online at: https://foobot.io/
